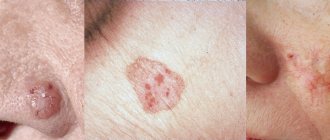
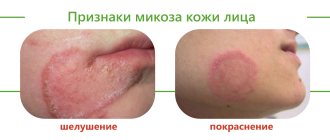
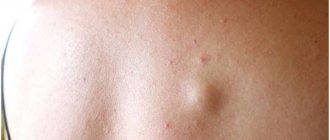
Effective procedures for the treatment of hyperkeratosis
Phototherapy
Plasma therapy
NeoGen procedure
Mesotherapy
Peeling
Medical pedicure
One of the fairly common types of skin diseases is hyperkeratosis. This is an excessive thickening of the stratum corneum of the epidermis. With the development of such a pathology, horn cells begin to rapidly divide and desquamation is impaired, which ultimately leads to thickening of the skin. Moreover, the thickening can reach several centimeters. According to statistics, hyperkeratosis is observed in approximately 20% of men and 40% of women. As a rule, the problem occurs in individual areas and leads to a significant deterioration in the appearance of the skin.
In children, the pathology can be observed at the age of 1–3 years, and it mainly affects the face and hands. In adults, changes in the stratum corneum are more common on the feet and toenails, as well as on the face and scalp. There are several types of the disease, which have their own symptoms and causes of development. Let's figure out what hyperkeratosis is and whether such a pathology is dangerous for health.
Classification
The classification of hyperkeratoses is based on a number of factors, according to which the following are distinguished:
- By origin: hereditary and acquired hyperkeratosis .
- By area of damage: local (calluses/warts) and diffuse, occupying large areas of the skin.
According to clinical forms:
- Follicular hyperkeratosis - in which exfoliating scales of the stratum corneum clog the ducts of the follicles, which is manifested by the appearance of numerous small tubercles on the skin.
- Seborrheic hyperkeratosis is localized mainly on the scalp, less often on the facial skin. It manifests itself in the formation of areas of peeling in the form of an easily detachable greasy crust, after which reddish spots remain.
- Warty hyperkeratosis . It is characterized by the appearance on the skin of formations that outwardly resemble warts, but without the etiological factor of true warts - papillomavirus .
- Hyperkeratosis of the feet . It manifests itself as thickening of the skin of the feet with the appearance of corns and calluses.
- Disseminated hyperkeratosis . It appears as polymorphic elements on the skin of the trunk and limbs, reminiscent of thick/short hair, located separately and not merging with each other.
- Lenticular hyperkeratosis . It is characterized by the appearance of horny papules on the hair follicles of the lower extremities, and after removal, small indentations remain on the skin.
- Senile hyperkeratosis . The appearance of dark keratinized spots on the skin of older people is typical.
Features of the pathology
The concept of hyperkeratosis comes from two Greek words: hyper – “many” and keratosis – “formation of keratin”. In fact, hyperkeratosis is not an independent disease - most often it is just a symptom of other diseases. For example, such a problem occurs with lichen, ichthyosis or erythroderma. However, thickening of the stratum corneum can sometimes appear in a healthy person: for example, the feet, elbows and knees are often susceptible to this problem.
Hyperkeratosis is considered a potentially life-threatening disease, but treatment is still recommended. Pathology can cause serious cosmetic defects, which often lead to social maladaptation and decreased self-esteem.
The basis of the stratum corneum of the skin is made up of horny plates, which contain the protein keratin. Typically, the layer includes 15–20 layers of horny scales; when the epidermis thickens, their number can reach 100.
Essentially, the stratum corneum is the end result of the division of keratinocytes of the epidermis, which is why it has a specific structure. It is based on horn cells held together by intercellular lipids. Normally, this layer of the epidermis is constantly renewed: the horny scales are peeled off and replaced with new cells.
The desquamation process starts in the basal layer of the skin, where keratinocytes are produced. After this, the cells gradually move to the upper layers, losing their nucleus and organelles and turning into flat scales, which develop into the stratum corneum.
Normally, the epidermal renewal cycle lasts about 21–28 days; with age it slows down and can reach 45–72 days. In addition, the state of cellular metabolism is influenced by various factors such as lifestyle, nutrition, and hormonal levels of the body.
With hyperkeratosis, the patient's production of proteolytic enzymes, which regulate the processes of destruction of protein bonds between the cells of the stratum corneum, is disrupted. As a result, there is no desquamation of old cells, and due to the accumulation of keratinocytes, a significant thickening of the epidermis occurs.
List of sources
- Bauman L. Cosmetic dermatology. Principles and practice. Per. from English Potekaeva N. N. M.: MEDpress-inform. 2012. 688 p.
- Afanasyev E.N. Mechanically induced hyperkeratoses of the foot // Plastic surgery and cosmetology. 2012. No. 4. pp. 644–661.
- Kholodilova N.A., Monakhov K.N. The use of basic care products in patients with impaired skin barrier // Russian Journal of Skin and Venereal Diseases. 2009. No. 6. pp. 68–69.
- Lomakina E. A. The role of the barrier function of the skin in the pathogenesis of some dermatoses // Modern problems of dermatovenereology, immunology and medical cosmetology. 2009, no. 2. pp. 87–90.
- Rodionov A. N. Dry skin. Dermatocosmetology. Lesions of the facial skin and mucous membranes. Diagnosis, treatment and prevention. SPb: Science and Technology. 2011. 911 p. pp. 63–69.
Types of pathology
The following forms of hyperkeratosis are distinguished:
- Follicular. This type of pathology is characterized by damage to the hair follicles. Most often, follicular hyperkeratosis appears in areas with dry, dehydrated skin. The reasons are heredity, vitamin deficiency, inflammatory skin diseases or neglect of personal hygiene. There are two forms of pathology: with follicular hyperkeratosis of type I, spiky nodules and plaques appear around the hair follicle, with type II - a hemorrhagic rash caused by a lack of vitamin C and K. Very often, the ducts of the hair follicles are clogged with blood or red pigment.
- Lenticular. This form is characterized by the appearance of small “plugs”, most often on the hair follicles, which look like keratinized spots. The reasons for the development are not exactly known, but most often the problem occurs in elderly patients. As a rule, the pathology is chronic, but without a tendency to regression.
- Disseminated. With this form, polymorphic elements appear on the skin, which outwardly resemble short and thick hair. They are isolated from each other and have no tendency to grow together.
- Seborrheic. This type of pathology is typical for oily skin and appears as a result of metabolic disorders. At an early stage, characteristic yellow-brown spots of a round shape appear, which gradually fade and turn into plaques. The lesions can be quite large in diameter.
- Warty. Externally, the warty form resembles warts, but their appearance is not caused by papillomavirus.
- Plantar. Hyperkeratosis of the feet can occur on the entire sole or only on the heel area. As a rule, this form is characterized by severe dryness and roughness of the skin, as well as noticeable thickening in the affected areas. There is a dry callus (a local lesion with clear boundaries of thickening of the stratum corneum), a core callus (a sharply limited area of thickening of a round shape of small size) and a soft callus (appears between the fingers as a result of increased humidity).
- Subungual. Quite often, subungual hyperkeratosis occurs, resulting from traumatic onychia or onychomycosis. It is characterized by rapid growth from the distal edge, which causes an enlargement of the nail plate.
Diagnosis and treatment of the disease
If characteristic skin problems appear, you should consult a dermatologist as soon as possible. The specialist examines the skin and collects the patient’s complaints. It is important to differentiate hyperkeratosis from other skin diseases, for example, psoriasis or lichen, which also cause peeling of the skin. If the diagnosis is in doubt, a biopsy of suspicious skin areas may be performed.
To treat the disease, ointments with topical corticosteroids are used to treat the damaged areas. This may include prednisolone or hydrocortisone ointment, fluacinolone-based formulations, or clobetasol. In addition, glucocorticoid drugs are prescribed, which have an exfoliating and anti-inflammatory effect, thoroughly cleansing and disinfecting the skin.
Patients with hyperkeratosis of any form are advised to take warm baths with the addition of salt, baking soda or starch and further moisturizing with cosmetic creams.
If hyperkeratosis is detected, mechanical peeling is contraindicated, as it can aggravate the patient’s condition. Only acid (chemical) peeling based on creams with a mild effect is allowed. These are products consisting of salicylic, lactic, citric and other acids. Vitamins A and C are also prescribed orally.
Plantar hyperkeratosis is treated with antifungal ointments, and also requires the elimination of all pathological factors of the disease. It is necessary to replace shoes with more comfortable ones, as well as receive orthopedic help in case of flat feet or club feet. In addition, salt baths, mechanical grinding using a hard sponge and pumice at home are useful. After this, the feet are lubricated with a moisturizing and nourishing cream.
As for possible complications of the disease, they can be observed with plantar hyperkeratosis, when cracks, corns appear, and a secondary fungal infection begins to develop. Follicular hyperkeratosis in some cases causes pyoderma. Formations with a warty form sometimes develop into a malignant tumor. The prognosis for timely and high-quality treatment of hyperkeratosis is favorable, although in some cases the fight against the disease can last a lifetime with alternating stages of exacerbation and remission.
Reasons for development
Pathogenesis varies depending on the specific type of disease. Very often, the development of pathology is facilitated by exogenous (external) causes. It could be:
- pressure on the skin;
- wearing uncomfortable clothes/shoes;
- exposure to aggressive agents.
This provokes the body’s protective functions, which, in turn, cause increased cell division. As a result, the natural process of cell desquamation is disrupted, which leads to a thickening of the skin layer.
The endogenous (internal) causes of the disease include the following factors:
- hereditary skin diseases;
- gastrointestinal diseases;
- disruption of the regeneration process after injury;
- skin neoplasms;
- fungal infections;
- hormonal imbalances;
- hypovitaminosis;
- inflammatory diseases;
- metabolic disorders in the body.
Excessive roughening of the skin is often explained by other ongoing diseases:
- psoriasis;
- ichthyosis;
- keratoderma;
- lichen;
- diabetes.
If we talk about foot hyperkeratosis, this form of pathology is often caused by improper gait or flat feet, excess body weight, and wearing tight and uncomfortable shoes.
Precancerous diseases of the red border of the lips (RBL) and oral mucosa (ORM)
I. K. Lutskaya
Doctor of Medical Sciences, Professor, Head of the Department of Therapeutic Dentistry BelMAPO (Minsk)
Diseases characterized by a high tendency to malignancy (obligate precancers of the oral mucosa and red border of the lips) require special consideration in dental practice. They are characterized by the absence of objective signs of a cancerous tumor, but in the presence of pathogenic factors they become malignant. The clinical manifestations of this group of diseases are quite diverse, which makes their diagnosis difficult. On the other hand, the prognosis depends on a number of factors, primarily the nature of the carcinogens, as well as the local status and general condition of the body. If adverse effects are excluded, reverse development of the lesion elements, stabilization of the process without significant changes, or further development without a tendency to degeneration are possible. The persistence of an unfavorable background leads to malignancy of the lesion.
The main signs of malignant degeneration can be the following symptoms: a sharp change in the clinical picture, namely acceleration of the development of a tumor or ulcer, exophytic growth or ulceration of the tumor (Fig. 1).
Rice. 1 a. Signs of malignancy.
Rice. 1 b. Signs of malignancy.
The next signal points are bleeding of the lesion, the appearance of hyperkeratosis, infiltration and compaction at the base (Fig. 2). The lack of effect of conservative treatment within 7-10 days is the basis for referring the patient for consultation to an oncologist or maxillofacial surgeon. Malignancy is confirmed by the results of morphological studies, namely the identification of atypical cells in the biopsy material.
Rice. 2. Bowen's disease.
Systematics of keratoses as precancerous conditions
I. Keratoses without a tendency to malignancy (initial form of leukoplakia, soft leukoplakia, geographic tongue, etc.).
II. Optional precancer with the possibility of malignancy up to 6% (flat form of leukoplakia, hyperkeratotic form of lichen planus; pemphigoid form of lichen planus, etc.).
III. Optional precancer with a tendency to malignancy (malignancy tolerance) from 6 to 15% (elevating form of leukoplakia; warty form of leukoplakia; erosive form of leukoplakia; warty form of lichen planus; erosive form of lichen planus; rhomboid glossitis - hyperplastic form, etc.).
IV. Obligate precancerosis with the possibility of malignancy over 16% (ulcerative form of leukoplakia; keloid form of leukoplakia; ulcerative form of lichen planus; follicular dyskeratosis; Bowen's syndrome; atrophic keratosis; xeroderma pigmentosa, ichthyosis vulgaris, etc.).
Bowen's disease
Bowen's disease has the highest potential risk of malignancy (Bowen, 1912), since its histological picture is cancer in situ (intraepithelial cancer without invasive growth). Clinical manifestations of Bowen's disease vary depending on the location, stage of the disease, and associated factors. The patient's complaints can be reduced to discomfort, roughness of the corresponding parts of the mucous membrane, more or less pronounced itching. In some cases, there are no subjective sensations, so the lesion will be detected during a routine examination of the oral cavity.
The favorite localization of lesion elements in the form of spots, papules, scales, erosions, and areas of keratinization are the posterior sections of the mucous membrane: the palatine arches, the root of the tongue. Clinical manifestations of the disease on the cheeks, lateral surface of the tongue, and soft palate are described. More often one, less often two or three areas of altered mucosa are found.
Most typical for the initial stages of the disease is the appearance of a limited area of hyperemia, which has a nodular-spotted or smooth appearance (Figure 3). A distinctive feature may be the peculiar velvety surface as a result of small papillary growths. The further clinical picture resembles leukoplakia or lichen planus due to the formation of areas of hyperkeratosis. There is a tendency to erosion. The lesion will rise above the level of surrounding tissues if nodules form and merge into plaques. With a long course, atrophy of the mucous membrane develops, and in such cases the affected area seems to sink.
Diagnosis is difficult when a small focus of hyperemia subsequently becomes covered with scales, resembling leukoplakia or lichen planus in appearance. The diagnosis of Bowen's disease is made on the basis of a histological picture: giant cells with an accumulation of nuclei in the form of lumps, the so-called monstrous cells, are found in the spinous layer.
The prognosis of the disease is unfavorable: the development of lesions within 2-4 months ends with invasive growth without a tendency to regression (reverse development).
Treatment for Bowen's disease involves complete excision of the lesion, which may include surrounding healthy tissue. In some cases, close-focus X-ray therapy is used.
Warty precancer
Warty precancer is an independent clinical form (A. L. Mashkilleyson). It is characterized by a pronounced tendency to malignancy: already 1-2 months after the onset of the disease. The patient's complaints boil down to the presence of a cosmetic defect and discomfort. The favorite localization of the lesion (usually single) on the red border of the lower lip allows for a detailed study of the clinical picture. The main element of the lesion is a nodule with a diameter of up to 10 mm, protruding above the level of the mucosa and having the usual color of the red border of the lips or a persistent red color (Fig. 4). The surface of the nodule may be covered with thin, tightly attached scales that cannot be removed when scraped. The tissue surrounding the lesion is not changed. Upon palpation, the compacted consistency of the nodule is determined, there is no pain.
Differential diagnosis with a wart, keratoacanthoma, papilloma is carried out on the basis of the clinical picture with mandatory pathological confirmation. Clinically, a common wart is characterized by a lobulated structure or papillary growths with a rim of stratum corneum along the periphery. Keratoacanthoma is characterized by a large number of keratinized cells filling the depression in the form of a funnel formed by a dense ridge of surrounding hyperemic mucosa. The papilloma has a stalk of soft consistency.
Treatment of warty precancer is only surgical with complete excision of the lesion and histological examination of the tissue. Confirmation of warty precancer is the proliferation of the epithelium due to the spinous layer both towards the surface and deep into the mucosa.
Rice. 3. Warty precancer.
Limited precancerous hyperkeratosis
As an independent disease, limited precancerous hyperkeratosis has a less pronounced degree of malignancy than warty precancer: the lesion can remain in a stable phase for months, even years. However, clinical signs of malignant degeneration are very unreliable, since increased keratinization processes, the appearance of erosion and compaction can be detected some time after the onset of malignancy. Therefore, the basis is histological examination. The patient makes no complaints or indicates a cosmetic defect. The characteristic localization of an area of altered polygonal mucosa on the red border of the lips makes it possible to diagnose limited hyperkeratosis. The grayish lesion may sink or rise above the surrounding unchanged red border without spreading to the skin or Klein's area (Fig. 5). The elevation of the lesion above the level of the lip is associated with the layering of scales, which cannot be removed when scraped. On palpation, the compaction at the base is not detected, but the dense consistency of the surface of the lesion is felt.
It is necessary to differentiate limited precancerous hyperkeratosis from leukoplakia, lichen planus, and lupus erythematosus. A diagnostic sign can be the lesion itself, which is small in size from a few mm
up to 1.5
cm
of polygonal shape with a tendency to form scales on the surface, which is not typical for leukoplakia. When localized on the lip, lichen planus is characterized by hyperemia, infiltration, whitish stripes, spots, and significant prevalence. With lupus erythematosus, inflammation, atrophic scars, and often erosion and diffuse damage to the red border are detected. Since histological examination is critical for the diagnosis of malignancy, biopsy should be performed as early as possible.
Treatment of limited hyperkeratosis consists of surgical removal of the lesion within healthy tissue; wedge-shaped excision is advisable. It is mandatory to exclude local irritants and bad habits: smoking, lip biting.
Rice. 4. Limited hyperkeratosis.
Abrasive precancrosis cheilitis Manganotti
The disease was first described by Manganotti (1913) and is considered in the group of obligate precancers due to its tendency to malignancy. It differs from other diseases of this group in its long course, tendency to regression (remissions), reappearance and development. Degeneration may occur after several months or many years.
A single lesion (rarely there are two) is localized on the red border of the lips in the form of oval or irregularly shaped erosion (Fig. 6). The surface of the erosion, having a bright red color, looks polished, can be covered with a thin layer of epithelium and does not tend to bleed. Drops of blood can be detected when crusts or crusts (serous, bloody) are separated, which can appear in the form of layers on the surface of erosions.
Rice. 5. Heilith Manganotti.
The element is localized on the unchanged red border of the lips. In some cases, congestive hyperemia and infiltration can be detected, but the background inflammation in Manganotti cheilitis is unstable.
Palpation does not detect changes in tissue consistency or pain. A feature of the clinical course of the disease is its intermittent nature: once it appears, erosion can spontaneously epithelialize, and then reappear in the same or another place, limited in size from 5 to 15 mm
.
It is necessary to differentiate Manganotti cheilitis from erosive-ulcerative forms of hyperkeratoses (leukoplakia, lichen planus, lupus erythematosus), herpetic lesions at the erosion stage, pemphigus, erythema multiforme. It is based on a characteristic picture of bright red erosion, often oval in shape, without bleeding or with the formation of bloody crusts on the surface. There are no lesions characteristic of hyperkeratosis in the form of spots, papules, stellate scars, or persistent hyperemia. In contrast to vesicular and vesicular lesions, fragments of blisters and specific cells are not identified (with pemphigus, herpetic stomatitis).
Erythema multiforme is characterized by an acute onset and pronounced prevalence of the process. Erosion in herpetic stomatitis is distinguished by scalloped edges as a result of the fusion of vesicles. If you have the habit of biting a portion of your lip, swelling and hyperemia are clearly visible, and signs of inflammation may transfer to the skin. Upon examination, individual point erosions or erosions merging into one are determined. Frequent lip biting confirms the traumatic nature of the disease. The history, as a rule, reveals a primary lesion in the form of a herpetic, mechanical, chemical, etc. lesion.
In doubtful cases, a histological examination is carried out, the diagnosis is confirmed by detecting epithelium infiltrated with histiocytes, lymphocytes, mast cells, as well as changes in the spinous layer and connective tissue.
Treatment of Manganotti cheilitis includes general and local treatments. Vitamins are prescribed internally to stimulate regeneration processes. Drugs that have an epithelializing effect are used locally: oil solutions of vitamins A, E, methyluracil, solcoseryl. In the presence of background inflammatory phenomena, it is possible to use corticosteroid ointments.
Conservative treatment of Manganotti cheilitis in the absence of signs of degeneration and a positive effect (the onset of stable remission) can last 2-3 months. Frequent recurrence, clinical growth, especially the appearance of the slightest signs of malignancy serve as an indication for surgical treatment (removal of the lesion within healthy tissue) with histological examination of the material.
Eliminating bad habits, irritating factors, and sanitation of the oral cavity are mandatory.
Tactics of a dentist
| Possible situations | Dentist tactics |
| Local manifestations in the presence of a local etiological factor: traumatic injuries, Vincent’s ulcerative necrotizing stomatitis | - diagnostics and treatment at the dentist — additional research is possible - therapy is usually local |
| Local manifestations in the presence of a common cause: chronic recurrent herpetic stomatitis, fungal infections, erythema multiforme | — diagnosis and treatment by a dentist after additional research and consultation with a specialist — local therapy, general therapy is possible |
| Local lesions against the background of general diseases: diseases of the gastrointestinal tract, cardiovascular system; allergic reactions, neurogenic and endocrine disorders; childhood infections, radiation sickness, myocardial infarction, blood diseases, tuberculosis, pemphigus | - dental examination — the final diagnosis is made by a doctor specializing in the field of this disease (hematologist, dermatovenerologist, allergist, etc.) - treatment by a specialist in the profile of pathology - general (etiotropic, pathogenetic), by a dentist - local, often symptomatic |
Particular vigilance should be exercised in cases of detection of a possible social risk or threat to the patient’s life. Depending on the specific clinical situation, the dentist bases his actions, including the following general rules.
- Each patient is admitted using personal protective equipment and sterile instruments.
- The initial examination of the oral mucosa is carried out only using instruments (mirror, probe, spatula, tweezers). Before special studies (serological, bacteriological, cytological) are carried out, the elements of the lesion are not palpated.
- In all doubtful cases, which include the primary detection of lesions on the mucous membrane or the lack of effect of treatment for a previously detected soft tissue change, the patient must be examined for syphilis and HIV infection. This recommendation is due to the fact that even a clinically clear local picture of the disease can accompany a general severe or infectious disease (for example, herpetic eruptions in AIDS, aphtha-like plaque in syphilis).
- Identification of positive serological blood reactions to syphilis or detection of Treponema pallidum in the lesion elements serves as an indication for treatment of the patient in a specialized institution. The situation is similar when identifying the causative agent of tuberculosis. HIV-infected people are served in AIDS centers, but they can also receive the necessary help from a dentist, which every outpatient doctor should remember.
- The initial detection of an ulcer with hardened edges or the lack of effect of treatment during an ulcerative process (7-10 days) requires consultation with an oncologist or maxillofacial surgeon, accompanied by a cytological or histological (biopsy) examination of the affected tissue. If signs of a tumor malignant process are detected, surgical treatment methods are used.
- A diagnosis confirmed by laboratory tests and excluding oncological or contagious diseases serves as the basis for prescribing conservative treatment, taking into account the etiology and associated factors.
General examination scheme
The first stage of interaction between a doctor and a patient is the collection of factual material, that is, the identification of symptoms of deviation from the norm. Next comes the clarification of the information received until the final diagnosis is made.
Research methods used in dentistry can be divided into the following groups: interviewing the patient (his relatives), examination, palpation, instrumental examination (probing, percussion of teeth, thermal diagnostics), assessment of gum and plaque condition indices, physical methods (electrical, radiological), laboratory studies (biochemical, bacteriological, cytological), special tests (blister test, histamine test, Kovetsky test, capillary resistance test), blood, urine, saliva tests.
Experts from the World Health Organization (WHO) recommend the following approach. The survey includes three parts: A
) extraoral region of the head and neck;
B
) perioral and intraoral soft tissues;
C
) teeth and periodontal tissues.
Settings, equipment and materials required (for all stages): adequate lighting, two dental mirrors and two gauze pads. We should not forget about gloves, a mask, and hygiene control.
The patient is in a sitting position.
First part of the examination - A
— requires a limited number of tools and takes no more than 5 minutes. The head, face, and neck are examined. The doctor evaluates changes in the size, color and shape of the parts of a given anatomical region.
When examining the skin, attention is paid to the presence of congenital changes (nevi, hemangiomas), as well as elements of damage in diseases. Notes the color, turgor, elasticity, moisture of the skin.
Some pathological changes, for example contractures, atrophy of facial muscles, are noticeable even during an external examination and must be recorded in the outpatient card (from a legal point of view, this is important in order to avoid a conflict situation when the patient is dissatisfied with the medical treatment provided).
It is necessary to pay attention to the shape and size of the pupils, which may reflect organic damage to the nervous system. Movement of the eyeballs is assessed, especially the presence of nystagmus (eye twitching). External examination of the facial muscles is insufficient. It is advisable to ask the patient to wrinkle his forehead, nose, open his mouth wide, and show his teeth. With facial nerve paralysis, tic-like twitching of the affected facial muscles, changes in the width of the palpebral fissure, and increased mechanical excitability of the muscles are observed. Peripheral paralysis of the lingual muscles causes fibrillary twitching with atrophy of the tongue (which may be a symptom of syringobulbia or amyotrophic lateral sclerosis). Bilateral paresis of the tongue causes a speech disorder such as dysarthria. Articulation defects and scanned speech are identified during conversation and questioning of the patient.
Part Two - B
- includes 7 steps: red lip border; mucous membrane and transitional fold of the lips; corners of the mouth, mucous membrane and transitional fold of the cheeks; gums and alveolar margin; language; floor of the mouth; hard and soft palate.
B1 - lips are examined with the mouth open and closed. The color, shine, and consistency of the red border are recorded.
B2 - examine the mucous membrane of the lips and transitional fold (color, consistency, moisture, etc.). Normally, small elevations are sometimes found on the inner surface of the lip due to small mucous glands, which is not a pathology.
B3 - using two mirrors, first examine the right, then the left cheek (mucous) from the corner of the mouth to the palatine tonsil (pigmentation, color change, etc.). Along the line where the teeth meet, there may be derivatives of the sebaceous glands, which should not be mistaken for a pathology. These pale yellow nodules with a diameter of 1-2 mm do not rise above the mucous membrane. It must be remembered that at the level of the 17th and 27th teeth there are papillae on which the excretory duct of the parotid gland opens, sometimes also mistaken for deviations.
B4 - gums: first examine the buccal and labial areas, starting from the right upper posterior area, then move along the arc to the left. They descend onto the lower jaw from the left back and move to the right along an arc. Then the lingual and palatal areas of the gums are examined: from right to left on the upper jaw and from left to right along the lower jaw. Discoloration, swelling and swelling of various shapes and consistencies may occur on the gums. Along the transitional fold there are fistulous tracts, which most often arise as a result of a chronic inflammatory process in the apical periodontium.
B5 - tongue: consistency, mobility, all types of papillae are assessed. The shape, size, color of the tongue, the nature of the location and development of the papillae are determined. A healthy tongue has a soft pink color, its back is velvety, clean, in the morning it is somewhat whitish due to keratinization of the filiform papillae. Deviations from the norm should be considered changes in the size of the tongue, the presence of plaque, areas of increased desquamation of the epithelium, swelling, erosion, excoriation, ulcers, changes in relief, various anomalies of shape, attachment of the frenulum, etc.
B6 - floor of the mouth: changes in color, vascular pattern, etc. are recorded.
B7 - palate: examined with the mouth wide open and the head tilted back; Use a wide spatula to carefully press the root of the tongue, and use a dental mirror to examine the hard and then the soft palate.
When characterizing lesions of the mucous membrane, they clarify the boundaries of the pathological focus (clear, fuzzy), the relationship of its edges with the surrounding tissues (at the same level, roller-shaped edges), color (white, gray, pink, yellowish, cyanotic), the nature of the surface of the lesion (moist, shiny , dull), surface relief (smooth, lumpy, covered with small papillary processes), vascular pattern (number, shape and diameter of capillaries, uniformity of vessels, their color, presence or absence of deformation, flask-shaped swelling, intermittency).
Third part - C
- includes examination of the dentition and periodontium.
C1 - first, all teeth are examined. Otherwise, the true cause may remain undetected if the pain radiates to a healthy tooth or there is a phenomenon of repercussion, complications or a combination of diseases. In addition, examination of the dentition during the first visit allows you to outline a general treatment plan, that is, sanitation, which is the main task of the dentist.
It is recommended to carry out the examination in the same order, according to a certain system, using a dental mirror and probe. The mirror allows you to examine poorly accessible areas and direct a beam of light to the desired area, and the probe allows you to check all fissures, depressions, pigmented areas, and defects. If the integrity of the enamel is not broken, then the probe glides freely over the surface of the tooth without getting caught in the grooves and folds of the enamel. If there is a carious cavity in the tooth, sometimes invisible to the eye, the probe gets stuck in it.
The occlusal and proximal surfaces are carefully examined and probed, on which it is quite difficult to detect a cavity, especially a small one.
The examination of the dentition ends with the registration of the dental formula in the outpatient card and the calculation of the CP with an analysis of its structure.
C2 - during periodontal examination, in addition to determining the condition of the gums ( see
. stage B4), describes the state of the dentogingival attachment.
Optimal determination of periodontal parameters is ensured by the study of special indices.
Symptoms of hyperkeratosis
The main symptom of the pathology (and its main characteristic) is thickening of the skin in the affected areas . Other symptoms may vary depending on the specific form of the disease.
With follicular hyperkeratosis, “goose bumps” appear, that is, dense reddish pimples with a spiky shape. They are located at the base of the hair follicles. Most often, all this is observed on the side or back of the thigh, buttocks, arms, and face. In rare cases, the patient may experience itching.
Plantar hyperkeratosis is characterized by roughening of the skin on the entire sole of the foot or only in the heel area. Calluses and bleeding cracks often occur, which causes discomfort and pain.
With the seborrheic form, characteristic pigmented formations appear, which over time lose color and become colorless plaques.
The symptoms of hyperkeratosis are more pronounced in adults; in children, the pathology is often similar to dermatitis. At the initial stages of development there are no symptoms.
Stages of development
The following stages of disease development are distinguished:
- First . In some areas, the skin turns pale and becomes dry. No thickening of the stratum corneum has yet been observed.
- Second. When touching the skin, particles falling off are noticeable. Slight thickening is possible.
- Third . The skin peels off greatly and loses its smoothness, becoming rough and rough to the touch.
- Fourth. At this stage, multiple complications arise that lead to serious changes in the appearance of the epidermis. The thickening of the stratum corneum is visible to the naked eye.