Quick transition Treatment of atopic dermatitis in children
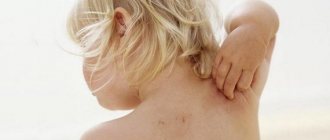
Atopic dermatitis is a disease in which the skin becomes very itchy, irritated, red, dry, and uneven.
Atopic dermatitis is a common skin disease that is part of a group of skin diseases combined under the broader term “eczema.”
There are other types of eczema: nummular, dyshidrotic, etc. However, the terms “eczema” and “atopic dermatitis” are often used interchangeably.
As a rule, atopic dermatitis debuts in infancy (3–6 months) and occurs in 15–20% of children. Most often, its course is most severe in the first 1–3 years of life; as the child grows older, the severity of the disease decreases. Atopic dermatitis usually disappears by school age or puberty. However, in some people the disease can persist throughout their lives, occasionally worsening, or appearing constantly.
What is atopic dermatitis
Atopic dermatitis is a chronic skin disease characterized by a relapsing course.
Babies with atopic dermatitis are bothered by itching and dry skin. Foci of inflammation can be located throughout the body, but they especially “love” children’s cheeks and folds, as well as the area under the diaper. Statistics indicate that atopic dermatitis occurs in every fifth baby [1]. Why is he dangerous? Lack of treatment can lead to the development of severe forms of atopic dermatitis, the spread of inflammation and the atopic march. In this condition, the disease begins to “march” through the child’s body, provoking the appearance or exacerbation of concomitant diseases. In 20-43% of cases, the development of bronchial asthma is possible, and twice as often - allergic rhinitis or eczema [2].
In addition, disruption of the hydrolipid barrier that occurs with atopic dermatitis in children can cause a secondary infection. Unfortunately, atopic dermatitis cannot be “outgrown.”
Treatment of streptoderma
Even if the initial examination was carried out by a pediatrician, a dermatologist should prescribe treatment for streptoderma in children.
A specialist in this profile is aware of narrow-spectrum drugs that will help to quickly cope with the disease. The first step is to transfer the child to a therapeutic diet with restrictions on sweets, fatty and salty foods. The course of therapy involves avoiding bathing: water procedures contribute to the spread of the disease. It is recommended to wash healthy areas with chamomile decoction, and never touch inflamed areas.
It is important to choose the right clothes for a sick child. Synthetic and wool items should be excluded from your wardrobe. These tissues cause discomfort and contribute to the spread of the disease.
Doctors recommend opening the blisters that form on the skin with a sterile needle, then treating the opening erosions with brilliant green 2 times a day. Areas of skin not infected with bacteria are wiped with a boron solution. Weeping erosions are lubricated with silver nitrate or resorcinol.
If crusts form on the skin, they are treated with antibacterial gels or ointments.
In severe cases, a number of other oral medications are prescribed:
- antibiotics of the tetracycline or chloramphenicol series;
- anti-allergy medications;
- immunostimulants;
- vitamin complexes;
- antipyretic drugs.
The list of medications must be agreed upon with your doctor. Only a specialist knows how to treat streptoderma in children correctly. Self-medication can provoke the pathology to become chronic. With an adequate course of therapy, the symptoms disappear after 7 days, but after curing the deep form of the pathology, scars remain on the skin. Therefore, it is necessary to consult a doctor as early as possible.
Symptoms of atopic dermatitis in children
According to recent studies [3], in 45% of babies, atopic dermatitis debuts between the ages of two and six months. In 60% of patients during the first year of life.
With atopic dermatitis in children, clinical symptoms and localization of inflammation largely depend on age. There are infant (up to one and a half years), child (from one and a half years to puberty) and adult phases. The following symptoms are common to all phases:
- Severe dryness of the skin (xerosis), which cannot be treated with regular baby cream .
- Redness and inflammation on the skin (especially symmetrical ones).
- Itching, causing severe discomfort to the child.
- Recurrent course (alternating periods of remissions and exacerbations). Moreover, in the cold season, deterioration is more often observed, and in the warm season, improvement is observed.
According to the nature of the course, acute and chronic stages of atopic dermatitis are distinguished, which are expressed by different signs (symptoms):
● Acute stage. Rough red spots (erythema), nodular rashes (papules), swelling, and crusts (including weeping) may appear on the baby's skin.
● Chronic stage. Accompanied by lichenification (thickening of the skin), cracks on the soles and palms, scratching, and increased pigmentation of the skin of the eyelids.
Allergic rash
In any case, parents are recommended to consult a doctor to determine the cause of the rash on the baby’s body. If a specialist discovers an allergy, then it is necessary to identify its form and irritant. Typically, the causative agent may be the following:
- the body's reaction to the weather (sun or cold);
- food allergies (in which the allergen product can be consumed by both the baby and the mother, if the former is breastfed);
- heredity (a child is at risk if at least one of his parents is predisposed to allergies);
- cosmetical tools;
- animal hair, dust, pollen;
- vaccination vaccines.
Once the cause of the rash is known, the next important step is to completely eliminate the irritant. It will be easier to do this in cases where the reason lies in external factors that they simply stop using (if they are creams, powders, detergents and other hygiene products). In the case where skin manifestations are the result of consuming certain products, it is important to exclude the product itself. The first signs may appear as early as an hour and a half after eating the allergen. Breastfeeding mothers must follow a diet and avoid spicy, fatty, chocolate, brightly colored fruits and vegetables, and alcohol. In such cases, it will be more difficult to get rid of the rash, since the product must be digested by the intestines, leave the baby’s body, and only after that the spots on the body will begin to disappear. You should know that when the pathogen reaches the baby through mother's milk, the process is delayed and recovery occurs after two weeks. Parents who themselves suffer from allergies should be extremely attentive to what their child is surrounded by and what he eats. Unfortunately, such babies are more prone to skin diseases than others. In this case, the irritant of an adult and an infant can be completely different. At the genetic level, only the predisposition itself is transmitted.
Almost always, allergies as a disease can be prevented. To do this, you will need to fulfill simple requirements:
- maintaining ideal cleanliness in the room, frequent wet cleaning and ventilation;
- introduction of complementary foods no earlier than four months from birth, and in some cases no earlier than six months. At the same time, it is important not to overdo it: if the introduced product is not suitable, then it should be offered to the baby again after one or two weeks;
- Diet compliance by a nursing mother. Drinking large amounts of liquid, broths and soups. Complete exclusion of harmful products;
- You should not self-medicate and try to prevent this or that reaction with the help of medications without appropriate doctor’s recommendations;
- maintaining hygiene and sharing a healthy lifestyle between mother and baby.
Walking in the fresh air, swimming, and hardening will have a positive effect on the health of all family members.
Urticaria and dermatitis are also types of allergic reactions. In the first case, there is a sudden appearance of itchy blisters on any part of the body. Such symptoms can occur from insect bites, from interactions with chemicals, and from eating strong allergens such as cow's milk, nuts, and honey. It is important to consider that prolonged exposure to the pathogen can worsen the baby’s condition, develop into edema and, at the same time, complicate breathing. Therefore, it is necessary to get rid of the presence of the irritant as quickly as possible and consult a doctor. Treatment occurs with the help of antihistamines and sedatives.
Dermatitis , like other types of allergies, is provoked by prolonged exposure to an irritant, increased sensitivity and predisposition to similar manifestations. Symptoms include inflammation of certain areas of the child’s skin (most often the hands, groin, cheeks), possibly burning and discomfort. Dermatitis is divided into several types:
- diaper (long-term interaction of delicate skin with irritants, such as wet diapers, diapers. Here you should change the diaper more often and wash the baby with running warm water before each change.
- Use wet wipes only when necessary, and apply a special protective cream under the diaper.);
- atopic (an outbreak occurs at the immune level, as the body’s response to respiratory and contact irritants. Localized on the cheeks, thighs, arms. Characterized by peeling lesions.);
- allergic (lack of vitamins in the body, consumption of allergic pathogens in food, lack of fresh air, moodiness, hyperactivity).
As in other cases, it is very important to make a diagnosis as quickly as possible and begin treatment in order to prevent transition to a chronic form. All allergenic foods should be excluded from the baby's diet; to reduce itching, the doctor will prescribe the use of a cream or ointment, and also prescribe the necessary medications to eliminate the causes. It is worth understanding that the problem always lies inside, and it is important not only to eliminate external symptoms, but also to completely destroy the original cause of the disease. When an allergy manifests itself against the background of vaccinations for a child, it is important to take into account the child’s predisposition in advance, notify the doctor about this and follow a number of measures prior to vaccination. Such events include the following:
- taking tests;
- use of antihistamines two to three days before vaccination;
- close observation on the day of vaccination and refusal of new products.
Parents need to know that any vaccine contains a potential pathogen. It can be chicken egg white, gelatin and other components that make up the drug. Therefore, after the vaccination has already been done, you need to stay with the child in a medical facility for about half an hour, in order to observe and take measures, if necessary. Most often, doctors do not recommend going for walks on the day of vaccination, especially if the baby is still very small and fragile. It will be necessary to monitor the general condition and possible changes for two weeks.
Rash caused by infections and viruses
Only a specialist can recognize the etiology of the formation of a rash on the baby’s skin and prescribe the need for treatment. But in cases where skin manifestations are accompanied by fever, stool disturbances, vomiting, and difficulty breathing, then most likely the nature of the disease is directly related to infection. Infectious rashes are caused by diseases such as:
- chickenpox (caused by the appearance of blisters containing liquid inside. The areas of spread itch and itch, and the temperature rises to critical levels. Throughout the maturation of the blisters, the child is a carrier of the infection. The affected areas are treated with brilliant green. If all the doctor’s instructions are followed, recovery occurs after 21 days.);
- rubella (this type of infection is characterized by cough, fever, enlarged lymph nodes, intestinal dysfunction, and, as a result, diarrhea and vomiting. The rash is usually not palpable, but appears in the form of redness of the skin. Most often, this disease occurs in children older than two years, but infants can also be infected, especially those who do not have the appropriate vaccination. The disease proceeds without complications and does not require special measures. It is only important to maintain bed rest and reduce the risk of rubella infection for other small family members, since five to seven days, an infected infant can infect unvaccinated children.);
- measles (the main reason for its appearance is the lack of vaccination. Infection occurs by airborne droplets, and symptoms begin to appear no earlier than a week later. As a result, it is not possible to notice the disease in time. Only after a few days do the symptoms of the disease make themselves felt : the temperature rises, a small rash appears first on the inside of the cheeks, head, and then throughout the body.The child’s immunity weakens, so it is necessary to feed it with vitamins during this period, and allow the body to cope with the disease on its own.
It is recommended to help the baby during this period, based on the symptoms that appear: antipyretics, throat sprays, nasal drops, as well as bed rest and frequent fluid intake. Treatment can take place both at home and in a hospital, under the supervision of a doctor, in order to eliminate the possibility of complications). A dermatologist or allergist will help you make the correct diagnosis. To do this, you need to undergo tests and, if necessary, skin scraping. An important role is played by external factors, the nature of the rashes, their localization, as well as the accompanying deterioration of the baby’s condition. In any case, it is necessary to follow all the doctor’s instructions regarding treatment and compliance with certain rules. The duration of allergies is also particularly influenced by the child’s immunity: the stronger it is, the sooner it will cope with the disease. Parents are required not to panic, but to notice the slightest manifestation of symptoms in time and contact a doctor as soon as possible.
Causes of atopic dermatitis in children
Atopic dermatitis can be considered a hereditary disease, because the most important role in its occurrence is played by a genetic factor [3]:
- In 80% of children, it occurs if both parents have or have had atopic dermatitis.
- In more than 50% of children - if at least one of the parents was sick, especially the mother (this doubles the risk of transmitting the disease “by inheritance”).
Some prenatal factors can also provoke atopic dermatitis in a baby: for example, poor nutrition of the expectant mother, contact with toxic substances, infections suffered during pregnancy, as well as bad habits and stress.
In addition, atopic dermatitis more often develops in babies who suffered oxygen deprivation during childbirth, were born prematurely and were bottle-fed (perinatal factors).
Diagnosis of atopic dermatitis in children
For a long time it was believed that atopic dermatitis in children is predominantly an allergic disease. However, it has now been proven that this is, first of all, a disease with dysfunction of the epidermis! And food allergies are detected only in 30-40% of children with atopic dermatitis.
The symptoms of atopic dermatitis are almost always influenced by certain environmental triggers. This could be chlorinated or “hard” water, soap, contact with an allergen, unfavorable climate and even stress. Another common trigger is bacteria that enter the skin through a damaged epidermal barrier.
Only a doctor (pediatrician, dermatologist, allergist) can make a diagnosis of “atopic dermatitis in children”! It takes into account the presence of external signs of disease and itching, as well as hereditary factors. Laboratory tests may be prescribed for children to carry out diagnostics. For example:
- General detailed (clinical) blood test.
- Biochemical general therapeutic blood test.
- General (clinical) urine analysis.
- Study of the level of total immunoglobulin E in the blood.
- Skin testing with allergens.
- Skin biopsy.
How to get rid of crusts on your face?
When dermatitis is localized on the face, the main rule remains the same: you should not pick off the scales with your fingernails or other sharp objects. Such actions can injure delicate skin and cause infection.
It is necessary to moisten the crusts with oil before each bath, and then carefully rinse with a delicate shampoo. Care must be taken to ensure that shampoo with oil residue does not get into the child’s eyes.
Since it is very problematic to comb out crusts from the face with a brush, it is recommended to simply wipe the affected area with a piece of clean flannelette cloth with slight pressure. The key factor in the fight against seborrheic dermatitis on the face is the regularity of procedures, and not the intensity of each of them. In the vast majority of cases, it is possible to avoid the formation of significant growths and completely get rid of unpleasant symptoms by 4-5 months of the baby’s life.
Treatment of atopic dermatitis in children
In modern medicine, there are three degrees of severity of atopic dermatitis in children:
- Easy. The child responds well to treatment, remission can last more than 10 months, the itching is minor, the redness is slight. Exacerbations occur no more than twice a year.
- Medium-heavy. Exacerbations occur 3-4 times a year, and periods of remission are reduced to 2-3 months. The therapy gives less pronounced results, the redness “stubbornly” returns.
- Heavy. Long-term exacerbations are interrupted by short periods of remission - up to one and a half months. Treatment helps little or for a short period of time; the baby’s behavior is greatly affected by itching [4].
At all stages of atopic dermatitis, pediatricians and dermatologists recommend emollients - cosmetic skin care products. They moisturize the skin and help restore the level of lipids - the most important structural components. During periods of exacerbation, emollients can be applied frequently and generously.
Pay attention to the composition; it is advisable that emollients are not addictive. Their main tasks are to help the skin produce its own lipids, providing effective hydration and softening. In addition, the constant use of emollients prolongs periods of remission and alleviates the symptoms of atopic dermatitis.
The Mustela Stelatopia line of cosmetics will help restore skin comfort for a long time! Stelatopia emollients are effective at all stages of atopic dermatitis , incl. at its first signs - increased dryness of the skin.
Studies have confirmed that the use of Stelatopia emollient cream can reduce the likelihood of developing atopic dermatitis by 51% ! [6]
Treatment (use of hormonal drugs) for atopic dermatitis in children can only be prescribed by a doctor, taking into account age, symptoms, concomitant diseases and test results. Self-medication can be dangerous!
- For external therapy for moderate and severe degrees of atopic dermatitis, topical glucocorticosteroids, topical calcineurin inhibitors and others are used.
- In case of mild disease, the use of Stelatopia Emollient Cream reduces the severity of inflammation after 32 hours, due to the presence of sunflower oil in the distillate [5].
- In systemic therapy, the drugs dupilumab, cyclosporine, glucocorticosteroids and others are used orally or in injection forms.
- To relieve itching - clemastine, hifenadine, cetirizine, chloropyramine, levocetirizine and others. The use of Stelatopia emollient cream as a cosmetic skin care product reduces the severity of itching in 80% of cases [7].
- Physiotherapy treatment may include phototherapy. Sometimes, in the treatment of atopic dermatitis, diet therapy, acupuncture, plasmapheresis and some other methods may be prescribed.
What to do if a child has diathesis
Local therapy using ointments is one of the components of complex treatment. But both hormonal and non-hormonal drugs should be prescribed by a doctor individually for each baby, taking into account the characteristics of the diathesis.
Self-medication in such a situation is not only ineffective, but also dangerous for the child’s health. Therefore, it is better to contact competent specialists. PsorMak employs doctors with extensive experience in treating diathesis.
We take a comprehensive approach to diagnosis and treatment, and for local therapy we use ointment made according to our own recipe without the addition of hormones.
She has been helping our patients at our clinic for more than 25 years, so we guarantee a complete cure without side effects. Contact us for a consultation so we can begin solving your problem. April 5, 2020
Author of the article: dermatologist Mak Vladimir Fedorovich
Prevention of atopic dermatitis in children
For atopic dermatitis, primary, secondary and tertiary preventive measures are distinguished.
Primary prevention
is aimed at preventing the occurrence of atopic dermatitis in children.
Recommended:
- Expectant mothers with a tendency to allergic reactions should exclude allergenic foods from their diet.
- Introducing complementary foods to babies begins at four months of age.
- Pregnant women and newborns at risk should take probiotics containing lactobacilli.
- Practice breastfeeding whenever possible.
- Eliminate exposure of your baby to tobacco smoke.
- Maintain humidity levels and regularly ventilate the children's room.
Secondary prevention
is aimed at eliminating risk factors that, under certain conditions (stress, weakened immunity, etc.) can lead to the occurrence, exacerbation and relapse of atopic dermatitis.
Recommended:
- Regular consultations with specialists.
- Maintaining awareness of new research and drugs in the treatment of atopic dermatitis.
3.Tertiary prevention
is a set of measures aimed at preventing exacerbations or development of complications of atopic dermatitis.
Recommended:
- Avoid contact of the baby with provoking factors: soap (it dries the skin), clothes made of rough or synthetic fabrics, low-quality cosmetics, etc.
- Take care of your child's skin and apply emollients on a regular basis, including during periods of remission.
- Bath your baby daily using cosmetic cleansers for atopic skin.
[1] Isaac Steering Committee. (1998). Worldwide variation in prevalence of symptoms of asthma. The Lancet, 351, 1225-1235. (International Committee on Asthma and Allergy in Childhood 1998. Worldwide differences in the prevalence of asthma symptoms. The Lancet, 351, 1225-1235). [2] Studies Watson W., 2011, Larsen F.S., 2002, Draaisma E., 2015, ISAAC Steering Committee, 1998. (Studies Watson W., 2011, Larsen F.S., 2002, Draaisma E., 2015 International Committee on the study of asthma and allergies in childhood, 1998). [3] Clinical guidelines. Atopic dermatitis, 2022. [4] Atopic dermatitis: recommendations for practitioners. Russian national consensus document on atopic dermatitis. Ed. P.M. Khaitova, A.A. Kubanova. M.: Pharmacus Print, 2002. 192 p. [5] ODT and inflammation June 2010 [6] Scientific dossier “Atopic-prone skin: latest discoveries” [7] Test report “Stelatopia” emollient cream, self-assessment by users
Prevention of childhood skin diseases
It is almost impossible to completely prevent the appearance of rashes on a child’s skin, but following simple rules will help reduce the risk of developing dermatological problems to a minimum.
How to avoid skin diseases:
- timely vaccination – vaccinations protect children from many viral diseases;
- regularly strengthen the immune system - hardening, following a daily routine, proper nutrition, exercise;
- observe the rules of hygiene;
- regularly carry out wet cleaning and ventilate the premises;
- immediately treat all wounds and scratches with antiseptic agents;
- take vitamin complexes twice a year;
- do not give your child antibiotics or other potent drugs without a doctor’s prescription;
- Regularly visit specialized specialists for preventive examinations.
Most skin diseases are contagious, sick children should be protected from communication with healthy ones, and they can only attend school and kindergarten if they have a certificate from a dermatologist.
Every child can develop skin rashes; the parents’ task is to contact a dermatologist in time to identify the cause of the disease, accurately follow all the doctor’s recommendations, keep the room clean, and follow hygiene rules.