ANESTHESIA IN THE DENTIST'S CHAIR OR, EVEN MORE, NARCASIS on the surgical table can be more frightening than the operations themselves: the injections are painful, and after general anesthesia you may not even come to your senses at all. Which of this is true and which is a myth, we’ll figure it out together with experts: a doctor of the highest category, anesthesiologist-resuscitator of the aesthetic medicine clinic “Time of Beauty” Oleg Karmanov, implantologist, orthopedist of the network of dental clinics “NovaDent” Mikhail Popov and anesthesiologist-resuscitator of the clinic “Refformat” Yuri Timonin.
How does anesthesia work?
Any anesthesia, local or general (the latter is also called anesthesia), is a medicinal intervention in the body that helps to avoid pain stress. In response to a pain impulse from the injured area, pain awareness occurs in the cerebral cortex. To prevent this, you need to block the nerve endings. Local anesthesia stops the transmission of pain impulses in a certain area - the medicine passes through the cell membranes and disrupts the reactions in them. As a result, nerve impulses are blocked and the sensation of pain does not occur. Consciousness is preserved during local anesthesia, and the effect lasts on average one to two hours. Anesthesia, or general anesthesia, is an effective method when a large area of the body is undergoing intervention. In this state, the person sleeps soundly and is well relaxed: tension in the muscles and other tissues should not interfere with the surgeon’s work.
Oleg Karmanov notes that it is wrong to be afraid of damage from the anesthetic: enduring pain is much more dangerous. In many cases, the risk of losing your life from painful shock during surgery without anesthesia is very high. According to the doctor, modern anesthetics are well controlled. This means that as soon as the active substance is no longer introduced into the body, it quickly disintegrates and the patient wakes up. The only absolute contraindication is an allergy to the drugs used, and possible side effects are usually associated with the presence of additional substances in the solution: vasoconstrictors (vasoconstrictors), preservatives and stabilizers.
Exudation
The alteration smoothly passes into the exudative phase, during which plasma and blood cells, tissue macrophages, leukocytes, etc. enter the cavities and/or intercellular space formed during the injury. Edema of the intercellular substance develops, in which active phagocytosis and a whole complex of biochemical reactions are still taking place, leading to the formation of exudate - a liquid very similar to blood plasma, but containing a large amount of protein, oligopeptides, whole and destroyed blood cells and tissues, etc. At this moment, patients often note: “Doctor, something is flowing from my wound!” This is the exudative phase of inflammation, a common, in general, stage of the postoperative period.
Another thing is that the nature of the exudate is an important sign of whether everything is in order with the postoperative wound. Most often, we observe serous or serous-fibrinous exudate - a translucent liquid of varying degrees of turbidity, slightly similar in taste and smell to blood. Such exudation is a normal phenomenon, indicating that everything is in order with the operation area, postoperative inflammation is proceeding as it should.
And sometimes nothing comes out of the wound at all - all the excess accumulates in the cellular spaces and cavities, gradually disappearing due to osmosis. This happens when we seal a postoperative wound, for example, during osteoplastic surgery.
In case of loss of control over the rehabilitation period, pus appears - exudate with a high content of protein, leukocytes, dead tissue cells and microbes. Its main difference between more or less acceptable wound discharge is its viscosity (very thick), transparency (opaque) and odor (unpleasant). The pus coming out of a postoperative wound does not pose any serious danger, because this is also a way of removing all sorts of nasty things from the body. As the nastiness becomes less, suppuration decreases and even stops completely. If pus, having formed, does not leave the wound or accumulates in the cellular spaces and cavities, this is already an abscess or phlegmon, which may require separate surgical treatment.
It is exudation that explains the increase in postoperative swelling on days 2-3 after surgery - at first, everything seems to look normal, but then the swelling increases, reaching its maximum, usually on days 2-3 - and many are very worried about this. Moreover, some patients evaluate the quality of the surgical treatment performed by the size of the resulting edema - they say, if there is no edema, then “the surgeon is great,” and if it is too large, then “the doctor did something weird.”
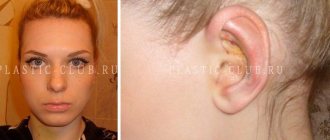
Meanwhile, the severity of edema is influenced by many factors, from the traumatic nature and duration of surgical intervention to the lability of the microvasculature, hormonal levels and the general condition of the body. And, unfortunately, it is not possible to reliably predict the size, period of formation and disappearance of edema. Look at the twins at the beginning of the article - it would seem that they are the same people and have the same operations - but how different the postoperative symptoms are!
In general, you need to know the following about the exudative phase of inflammation:
– there is always exudation, even when “nothing flows” from the wound. Swelling of the postoperative wound area is explained, among other things, by the accumulation of exudate in the soft tissues.
– not every exudate is pus. The flow of fluid from a wound is not at all a reason to undo the stitches and immediately pick and rinse something there. In itself, exudation is not dangerous.
– purulent exudate does not form immediately after surgery. It takes time for pus to form. Therefore, if your cheek is swollen after surgery, this does not mean that there is pus there.
– swelling of soft tissues is not necessarily a “flux” in the popular sense of the word or a phlegmon (abscess) in the medical sense. If the postoperative period is favorable, it passes within a few days. Only a doctor can catch the moment at which “something goes wrong” - that’s why it is important to be monitored after surgery.
– the severity and magnitude of postoperative edema are difficult to predict due to the many factors influencing them.
– the size and severity of edema cannot be used to judge the quality of the surgical treatment performed.
In addition to removing inflammatory agents from the body, the exudative phase has another important function; it facilitates the migration of cells and biologically active substances that trigger the next phase of inflammation - proliferation.
How to prepare for surgery under anesthesia and why it can be bad after it
Depending on the type of intervention, you need to undergo prescribed examinations - usually blood tests, an ECG, and sometimes, for example, an ultrasound of the lower extremities, to exclude the presence of blood clots - and also stop drinking alcohol and taking certain medications for a certain time before the operation. If the test results satisfy the doctor, he will confirm the planned operation. In this situation, drugs with a mild effect are used and recovery from anesthesia is usually painless. It is worth considering that during the operation processes such as changes in blood pressure may occur - but the work of the anesthesiologist does not stop after the patient is put under anesthesia; During the entire operation, the doctor monitors the depth of anesthesia and brain activity. The so-called neuroprotection is also used - protecting nerve cells with the help of certain medications.
Karmanov notes that unpleasant consequences after recovery from anesthesia—memory impairment, absent-mindedness, hallucinations—usually occur during emergency operations when you need to act very quickly, for example, after a large loss of blood as a result of a car accident. In these cases, drugs with a hypnotic, that is, hypnotic, effect are used, which can give such side effects. With special care, the doctor should also select drugs for pain relief for those who have cardiovascular diseases, problems with the respiratory system, kidney failure, hormonal disorders and diabetes.
Contraindications to the use of Propofol
The drug cannot be used by everyone. Absolute contraindications for the use of Propofol are:
- presence of allergies to the components of the drug,
- children's age up to 1 month.
It is also not recommended to use Propofol during pregnancy, because it penetrates the placental barrier. During the feeding period, the use of the medicine is allowed, provided that the woman does not feed for several hours after using the drug.
Relative contraindications for Propofol:
- serious diseases of the cardiovascular system,
- respiratory diseases,
- pathologies of the liver and kidneys,
- anemia,
- epilepsy,
- lipid metabolism disorders.
In all these cases, consultation with a specialized doctor is necessary. In case of stable remission of the disease, in the absence of a conflict between Propofol and the medications taken by the patient and some other circumstances, the doctor may authorize the use of Propofol.
Is it true that you can wake up during anesthesia or not wake up after?
It is theoretically possible to wake up during an operation if the dosage is incorrectly calculated, the anesthetic is selected incorrectly, or the body itself processes the injected drugs too quickly. But in practice this is extremely rare. Usually the doctor monitors the situation well and knows when a “supplement” of the drug is needed so that the patient’s sleep remains restful.
There is also a risk of not waking up after an operation performed under anesthesia, but experts note that the likelihood of death is high only in emergency and neurosurgery. True, in these situations, death more often occurs not because of anesthesia, but because of a serious condition - an acute injury or a life-threatening illness. In the case of planned operations, the probability of not surviving due to the fault of anesthesia is close to zero. In general, if the technique is followed and the necessary control is provided, anesthesia does not pose a threat to health, much less life.
What is sedation and why is it needed?
Sedation is the intravenous administration of non-narcotic hypnotics that induce shallow sleep. It is used for various types of endoscopy, for colonoscopy, but most often in the dentist’s office. When a person is dozing, light contact with him is possible: vital reflexes and body functions are preserved and the patient responds to the doctor’s requests, for example, to turn his head or “bite a piece of paper.” Sedation is accompanied by local anesthesia to numb the work area itself.
According to anesthesiologist Yuri Timonin, propofol does not cause side effects, and the substance itself has a short-term effect and is quickly eliminated from the body. The big advantage of sedation is that it allows you to increase the treatment time to 3.5–4 hours, without stress for the patient, with easy awakening and no unpleasant consequences after it. Doctors recommend this method for arterial hypertension and angina pectoris, as well as for those who are afraid of dentists to the point of losing consciousness.
What group of drugs does Propofol belong to?
Propofol is a drug whose purpose is to induce and maintain general anesthesia, as well as sedation during mechanical ventilation. Chemically, Propofol (more precisely, its main active ingredient diisopropylphenol) is a phenol molecule with two isopropyl groups attached to it. It is not included in the groups of barbiturates or opioids, it is not a narcotic drug, therefore it is not characterized by the severe side effects of drugs from these groups.
Is dental anesthesia safe during pregnancy?
Implantologist Mikhail Popov emphasizes that local anesthesia not only does not threaten the health of the fetus, but is also recommended for dental treatment, especially in the second and early third trimester of pregnancy. The anesthetic is absorbed into the blood in minute quantities and does not penetrate the placenta, so it will not affect the course of pregnancy and the condition of the fetus. Yuri Timonin adds that local anesthesia allows you to “turn off” a fairly large area of the jaw associated with the blocked nerve for 1–1.5 hours. Moreover, the harm from it is always less than from the source of infection in the mouth.
Women should warn the dentist about pregnancy before starting treatment: this information will allow them to make a choice in favor of drugs without adrenaline, which are best suited for expectant mothers. It is worth postponing the solution of non-urgent dental problems at 35-40 weeks of pregnancy - but in case of urgent treatment, for example, for inflammatory processes and ulcers, local anesthesia is given throughout the entire pregnancy. As for sedation, this method is contraindicated in pregnant women: the effect of drugs on the fetus has not been fully studied.
Use of propofol
Medication-induced sleep during dental treatment is used in several cases. First of all, this is dental phobia - a pathological fear of dental treatment. This is not just a fear that a strong-willed adult can cope with. As a rule, this is a series of involuntary nervous and physiological reactions that a person cannot control. In addition, a long complex operation, even in the absence of pain, often causes stress and deterioration of physical condition - increased stress on the heart and vascular system, exacerbation of chronic diseases, etc. Therefore, indications for the use of Propofol include:
- dental phobia,
- long operations with a high level of injury,
- increased sensitivity to pain,
- inability to establish contact with a doctor in some patients.
The drug is used to induce medicinal sleep in both adults and children, and even children under 1 year of age are not an obstacle.
Epidural anesthesia: pros and cons
Thanks to epidural anesthesia, when an anesthetic is injected into the space along the spinal canal, contractions become less painful and labor is noticeably calmer - while the woman is conscious. With a good dose calculation, sensitivity disappears almost only in the pelvic area, but sensations in the legs and the ability to move them remain. This anesthesia is also called walking epidural, although in fact you won’t be able to walk - your legs will be weak, and sensors or catheters on different parts of the body will not allow you to go far. The psychological aspect is also important: when you know in advance that it won’t hurt, it’s much easier to relax and not worry.
According to Oleg Karmanov, with epidural anesthesia already performed, it is faster and easier to proceed to an emergency caesarean section, if necessary: you will not have to waste time on pain relief. But you can’t always rely on epidural anesthesia; at a certain stage of labor it is already too late to perform it. The method has a number of contraindications, including intervertebral hernia and serious circulatory and coagulation disorders. Dangerous complications of epidural anesthesia are extremely rare.
What to expect from anesthesia in the future
The main feature of modern anesthetics is good controllability. Once the supply of the drug is stopped, it begins to quickly disintegrate. As a result, it is convenient for the doctor to control the time and depth of anesthesia for different conditions: the anesthesiologist will select one mixture of drugs for a patient with heart disease, and another for a person with respiratory tract disease. In both cases, it will be anesthesia with minimal drug load on the body. At the same time, various anesthesia devices, such as modern intravenous catheters, increase safety and comfort during surgery. Careful monitoring of the patient’s condition (measurement of pulse, blood pressure, amount of oxygen in the blood automatically) is another bonus of general anesthesia in modern conditions.
New generation local anesthetics have much fewer side effects and contraindications compared to drugs even ten years ago, and the waiting time for an effect has been reduced to five minutes. Doctors agree: over time, the percentage of allergic reactions will become zero, and the injection itself will be completely painless. The controllability of the process during anesthesia will also increase: it will become possible to bring a person in and out of a state of deep sleep even faster, as well as return him to consciousness at any appropriate moment. Oleg Karmanov does not rule out that in the near future, instead of intravenous anesthesia, a drug in the form of a pill will appear: he ate the pill and fell asleep.
True, anesthesiologists will still not be left idle: the patient’s condition is very important to constantly monitor and correct correctly. But whether it will be possible to replace anesthesia with hypnosis is a big question. In 2006, British television showed an operation to remove a stomach tumor under hypnosis, without the use of anesthesia, and in 2008, in one of the Iranian clinics, a hypnotized woman was successfully performed a caesarean section without anesthesia. However, Mikhail Popov notes that, despite the emerging information about such cases, there is no scientific research on this topic yet.
Proliferation
Yessss! We all live and work for proliferation. This is the most anticipated phase of inflammation for any surgeon. It is characterized by the migration of cells and the biologically active substances that control their division and differentiation, as well as the launch of regeneration processes of damaged tissues. In fact, proliferation very smoothly turns into regeneration, which, in principle, is the basis of such treatments as bone tissue augmentation, implantation and gum surgery.
During the proliferative phase, active movement of precursor cells (fibroblasts, osteoblasts) occurs. This movement is controlled by hormone-like substances (about thirty compounds in total, the most famous group for dentists are bone morphogenesis proteins, BMP-I, BMP-II), formed during the previous phases of inflammation. In parallel with migration, the processes of division and differentiation of cells already located in the area of injury and surgery are launched.
In fact, proliferation is the beginning of the regenerative process, with the help of which our body restores its integrity, and at the same time integrates implants and biomaterials. We have talked about regeneration many times, for example, here>>, here>> and here>>, and we will talk a lot more as we study osteoplastic surgery and implantation. And we will consider it as a separate process, in which inflammation is just a starting point, an initiator, nothing more.
Unfortunately, not all tissues are capable of proliferation. Thus, nerve fibers practically do not regenerate, but they have good intracellular restoration capabilities (hyperplasia and hypertrophy). The proliferation rate of different tissues and cells also differs: for example, connective tissue itself regenerates much faster than bone tissue, therefore, when growing bone tissue, in order to avoid growth into the graft, we separate it with a barrier membrane. Read more about this here>>
You need to know the following about the proliferative phase:
– proliferation will not occur without the two previous stages of inflammation, alteration and exudation. In other words, there is no creation without prior destruction.
– all components necessary for proliferation appear in the postoperative wound , thanks to the two previous phases of inflammation.
– in general, proliferation requires cells and substances that control the migration, division and differentiation of these same cells.
– proliferation can be considered as the initial stage of regeneration. It turns out that there is no regeneration without an inflammatory process preceding it.
– proliferation is a nonlinear process. Over time, the rate and intensity of proliferation slows down.
– it is impossible to control proliferation. Almost impossible. Cells cannot be forced to migrate, divide, and differentiate faster than nature intended. The maximum that we, doctors, can do is to calmly and confidently guide the patient through the two previous phases of postoperative inflammation, so that proliferation also occurs calmly and confidently.